Major Health Breakthrough: At-Home HPV Tests Poised to Revolutionize Cervical Cancer Screening Nationwide
New federal screening guidance has significantly expanded options for cervical cancer testing across the United States, introducing a widely accessible at-home Human Papillomavirus (HPV) self-collection method. This landmark update, issued recently, aims to overcome long-standing barriers to preventative care, potentially transforming how millions of individuals access critical health screenings nationwide.
The move represents a pivotal shift in public health strategy, leveraging convenience and privacy to boost screening rates, especially among underserved populations.
Background: The Evolution of Cervical Cancer Prevention
Cervical cancer is primarily caused by persistent infection with high-risk types of the Human Papillomavirus (HPV). For decades, the Papanicolaou (Pap) test, introduced in the 1940s, served as the cornerstone of screening, detecting abnormal cervical cells before they progressed to cancer.
In the early 2000s, HPV testing gained prominence, with the U.S. Food and Drug Administration (FDA) approving tests to detect the virus directly. This led to "co-testing" (Pap test combined with HPV test) and eventually, primary HPV testing as recommended options for certain age groups, particularly women aged 30-65.
Despite these advancements, significant disparities in screening rates have persisted across the United States. Barriers such as geographic distance, lack of insurance, cultural factors, fear of pelvic exams, time constraints, and limited access to transportation have prevented millions from receiving timely screenings. Rural communities, low-income populations, and certain racial and ethnic minority groups have historically faced higher rates of cervical cancer due to these systemic challenges.
Leading organizations like the U.S. Preventive Services Task Force (USPSTF) and the American Cancer Society (ACS) have continually refined their guidelines based on evolving scientific evidence. The concept of HPV self-collection has been studied extensively for over a decade, with numerous clinical trials demonstrating its accuracy and acceptability, paving the way for its eventual endorsement by federal health authorities.
Key Developments: At-Home Testing Becomes a National Option
The recent federal guidance now formally integrates at-home HPV self-collection as a recommended option for cervical cancer screening. This pivotal change is backed by robust clinical evidence and aims to democratize access to preventive care, particularly for individuals who are overdue for screening or face significant barriers to clinic-based testing.
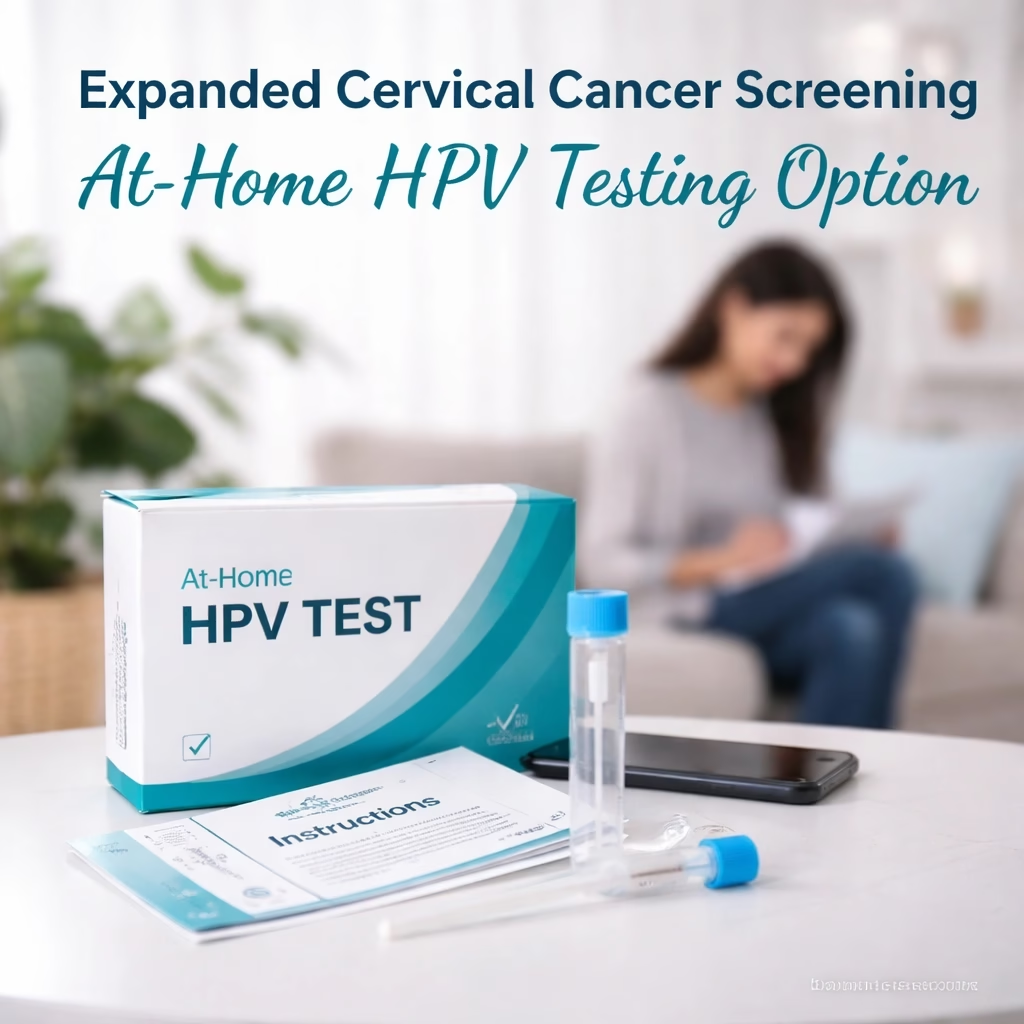
The at-home process involves a self-collection kit, typically mailed directly to the patient's residence. The individual collects a vaginal sample using a simple brush or swab device, following clear instructions provided with the kit. The sample is then securely mailed back to a certified laboratory for analysis, where it is tested for high-risk HPV DNA using highly sensitive molecular methods.
This method offers several distinct advantages. It provides an unprecedented level of convenience, allowing individuals to perform the test privately in their own homes, eliminating the need for a clinic visit. This reduces logistical hurdles such as taking time off work, arranging childcare, or securing transportation. Furthermore, it addresses discomfort or anxiety associated with traditional pelvic examinations, which can be a significant deterrent for many.
The FDA has played a crucial role by approving specific HPV self-collection devices and associated laboratory tests, ensuring the accuracy and reliability of these new screening tools. While not replacing conventional Pap tests or clinician-collected HPV tests, this option expands the toolkit for cervical cancer prevention, making screening more accessible to a broader segment of the population.
Impact: Reshaping Public Health and Patient Experience
The integration of at-home HPV testing is poised to have a profound impact across multiple facets of the healthcare landscape, from individual patients to national public health outcomes.
Enhanced Patient Access and Empowerment
For patients, the most immediate benefit is increased convenience and privacy. Individuals who have delayed or avoided screening due to discomfort, fear, lack of time, or geographic isolation can now access a critical preventive service. This empowers individuals to take a more active role in their health management, reducing anxiety and overcoming long-standing logistical barriers. It is particularly impactful for those in rural areas, individuals with disabilities, or those with limited access to transportation or paid time off.
Transforming Healthcare Provider Workflows
Healthcare providers will experience new workflows and responsibilities. While the initial collection is self-managed, providers will be crucial in ordering kits, educating patients on their proper use, and most importantly, ensuring timely follow-up for positive results. A positive HPV test from an at-home kit still necessitates a clinic visit for further evaluation, such as a colposcopy and biopsy, to detect and treat any precancerous lesions. This requires robust communication channels and patient navigation strategies.
Addressing Health Disparities and Reducing Cancer Burden
From a public health perspective, this guidance holds immense potential to significantly reduce the incidence and mortality rates of cervical cancer. By expanding access, it directly addresses health disparities that disproportionately affect underserved populations, including racial and ethnic minorities, uninsured individuals, and those in geographically isolated communities. Increased screening rates mean more precancerous lesions can be detected and treated early, ultimately preventing invasive cancer and saving lives.
Economic and Systemic Considerations
The economic impact is multifaceted. While there are costs associated with kit distribution and lab processing, these may be offset by reduced costs from treating advanced-stage cancers. Furthermore, under the Affordable Care Act (ACA), preventive services are typically covered without cost-sharing, which should facilitate widespread adoption once insurance policies are fully aligned. Health systems will need to adapt their infrastructure to support the logistics of kit distribution, sample return, and seamless integration of results into electronic health records.
What Next: Implementation and Future Horizons
The successful integration of at-home HPV testing into national screening programs will require a concerted effort from various stakeholders. Several key milestones and considerations lie ahead.
Robust Public Awareness and Education Campaigns
Widespread public awareness campaigns are essential to inform eligible individuals about this new screening option, its benefits, and the critical importance of follow-up for positive results. Organizations like the Centers for Disease Control and Prevention (CDC) and the American Cancer Society will play a vital role in disseminating accurate, culturally sensitive information. Simultaneously, healthcare providers will need comprehensive training on how to counsel patients, order kits, and manage the new screening pathway effectively.
Standardization of Insurance Coverage and Logistics
Consistent and comprehensive insurance coverage by Medicare, Medicaid, and private insurers will be crucial for equitable access. Clear policies on reimbursement for the kits and associated lab processing must be established. Logistically, robust systems for kit distribution, secure sample return, and efficient laboratory processing will need to be scaled up across the country to meet anticipated demand.
Integration with Healthcare Information Systems
Seamless integration of at-home HPV test results into existing electronic health record (EHR) systems is paramount. This will ensure that patient records are complete, follow-up recommendations are triggered appropriately, and population-level screening data can be effectively monitored to track progress and identify areas for improvement.
Ongoing Research and Policy Evolution
Future research will continue to evaluate the long-term impact of at-home HPV testing on screening adherence rates, cervical cancer incidence, and cost-effectiveness. Studies may also explore optimal screening intervals for self-collection and its potential integration with telemedicine models. As real-world data emerges, federal guidelines may be further refined to optimize the program’s effectiveness.
Broader Implications for Self-Collection Technologies
This significant advancement in cervical cancer screening could also pave the way for the broader application of self-collection technologies for other preventive health screenings, such as colorectal cancer or certain sexually transmitted infections. The success of at-home HPV testing may serve as a blueprint for future innovations in accessible, patient-centered healthcare, marking a new era in public health prevention strategies.