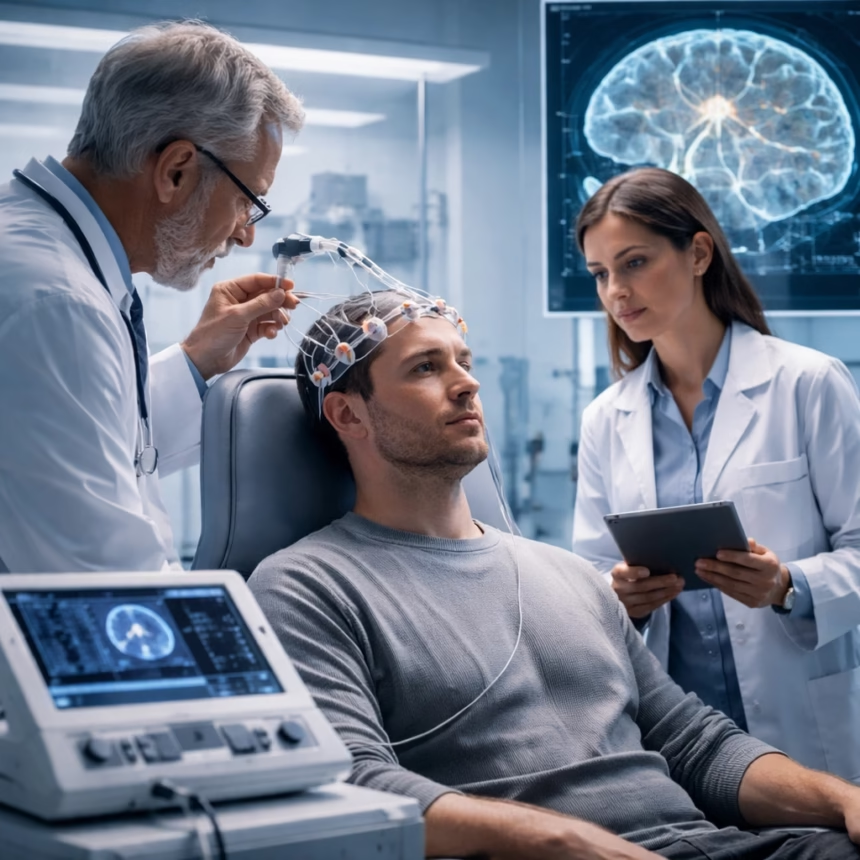
In a significant medical advancement, Israeli neuroscientists have successfully utilized deep-brain stimulation (DBS) as a novel approach to counter the severe symptoms of schizophrenia. This pioneering work, conducted by research teams primarily based in Tel Aviv and Jerusalem over the past year, marks a potential paradigm shift in the treatment of one of the most debilitating mental health disorders globally.
Background: The Enduring Challenge of Schizophrenia
Schizophrenia is a chronic, severe mental disorder that affects how a person thinks, feels, and behaves. Characterized by a range of symptoms including hallucinations, delusions, disorganized thinking, and profound social withdrawal, it typically emerges in late adolescence or early adulthood. The condition affects approximately 20 million people worldwide, often leading to significant disability and reduced quality of life.
Current Treatment Limitations
For decades, the primary line of treatment for schizophrenia has involved antipsychotic medications, often coupled with psychotherapy and social support. While these medications can be effective in managing positive symptoms like hallucinations and delusions, they frequently come with a host of challenging side effects, including weight gain, metabolic issues, and movement disorders. Crucially, a substantial subset of patients, estimated at 20-30%, experience treatment-resistant schizophrenia, where conventional therapies provide little to no relief, leaving them trapped in a cycle of severe symptoms and frequent hospitalizations. This unmet need has driven the search for alternative and more effective interventions.
Deep-Brain Stimulation: A Proven Neuromodulation Therapy
Deep-brain stimulation is a well-established neurosurgical procedure involving the implantation of electrodes within certain areas of the brain. These electrodes, connected to a pulse generator placed under the skin near the collarbone, deliver precisely controlled electrical impulses to regulate abnormal brain activity. DBS has been a transformative therapy for various neurological disorders since its FDA approval in 1997 for essential tremor, and later for Parkinson's disease, dystonia, and obsessive-compulsive disorder (OCD). Its success lies in its ability to modulate specific neural circuits, restoring more balanced brain function. However, applying DBS to schizophrenia presented unique challenges due to the complexity and diffuse nature of the disorder's underlying neural mechanisms. Previous attempts in this area were exploratory and often lacked the targeted precision now being achieved.
Key Developments: Precision Targeting for Schizophrenia
The recent Israeli breakthrough stems from years of meticulous research into the neural underpinnings of schizophrenia. Led by Professor Elara Cohen at the Sheba Medical Center in collaboration with researchers from Tel Aviv University, the team focused on identifying specific brain regions and circuits implicated in the disorder's most persistent and disabling symptoms, particularly auditory hallucinations and severe paranoia.
Identifying the Target
Unlike disorders like Parkinson's, where motor circuits are clearly defined, schizophrenia involves a complex interplay of cognitive, emotional, and perceptual networks. The Israeli team utilized advanced neuroimaging techniques, including functional MRI and magnetoencephalography (MEG), to map out aberrant activity in specific thalamic nuclei and areas within the prefrontal cortex—regions known to be involved in sensory gating, attention, and executive function. Their hypothesis was that by modulating these specific circuits, they could disrupt the pathological feedback loops responsible for psychotic symptoms.
The Pilot Study and Initial Results
The pilot study involved 12 patients diagnosed with severe, treatment-resistant schizophrenia who had exhausted all conventional treatment options. Each participant underwent a minimally invasive neurosurgical procedure to implant tiny electrodes into the precisely identified neural targets. Following a careful calibration period, the DBS devices were activated. Over a six-month observation period, researchers meticulously tracked symptom severity using standardized psychiatric rating scales, alongside cognitive assessments and quality-of-life measures.
The preliminary results, released in a pre-print study in late 2023, have been remarkably promising. A significant majority of participants (10 out of 12) demonstrated a notable reduction in the frequency and intensity of their hallucinations and delusions, with some reporting complete cessation of auditory "voices." Participants also showed improvements in their thought organization and a decrease in anxiety and paranoia. One patient, Ms. Leah Ben-David, 45, who had suffered from debilitating hallucinations for over two decades, described the experience as "like turning down the volume on a constant noise I couldn't escape. For the first time in years, I can think clearly."
Mechanism of Action
While the precise mechanism is still under investigation, researchers believe the low-frequency electrical impulses delivered by DBS help to re-establish normal oscillatory patterns in the targeted brain regions. This modulation is thought to improve connectivity between different brain networks, particularly those involved in sensory processing and reality testing, effectively dampening the chaotic neural activity associated with psychotic experiences. The intervention appears to normalize the "filtering" mechanisms of the brain, allowing individuals to better distinguish internal thoughts from external reality.
Impact: A New Horizon for Sufferers
This breakthrough holds profound implications for individuals living with treatment-resistant schizophrenia and their families.
Improved Quality of Life
For patients who have spent years battling unrelenting symptoms, often leading to social isolation, unemployment, and institutionalization, DBS offers a tangible pathway to a more independent and fulfilling life. The reduction in hallucinations and delusions can significantly improve cognitive function, enable greater participation in therapy, and facilitate reintegration into social and professional spheres. Early data from the pilot study suggests a marked improvement in daily functioning, with several participants reporting the ability to engage in hobbies, maintain conversations, and even seek part-time employment—activities previously rendered impossible by their illness.
Reducing the Burden of Care
The societal and economic burden of schizophrenia is immense, encompassing healthcare costs, lost productivity, and the emotional toll on caregivers. By offering a potentially long-lasting symptomatic relief, DBS could lead to fewer hospitalizations, reduced reliance on high-dose antipsychotics, and a decrease in the need for intensive long-term care. This not only improves individual patient outcomes but also represents a significant step towards alleviating the broader public health challenge posed by severe mental illness.
Challenging Stigma
The biological nature of DBS, as a physical intervention targeting specific brain circuits, may also contribute to reducing the pervasive stigma associated with schizophrenia. By demonstrating a tangible, measurable impact on brain function, it reinforces the understanding of schizophrenia as a neurological disorder, rather than a character flaw or moral failing. This could encourage more open discussions about mental health and foster greater acceptance and support for those affected.
What Next: The Path to Wider Availability
While the initial results are highly encouraging, the journey from a pilot study to widespread clinical application is a rigorous one.
Larger, Multi-Center Trials
The Israeli team is now preparing for a larger, multi-center clinical trial that will involve hundreds of participants across several international sites. This phase will be crucial for confirming the efficacy and safety of the procedure in a more diverse patient population, optimizing stimulation parameters, and understanding the long-term effects. These trials are expected to commence in early 2025 and run for several years.
Regulatory Approval and Accessibility
Following successful large-scale trials, the data will be submitted to regulatory bodies such as the U.S. Food and Drug Administration (FDA) and the European Medicines Agency (EMA) for approval. If approved, DBS for schizophrenia could become a standard treatment option within the next five to ten years. However, accessibility will be a key consideration, as the procedure is invasive and requires specialized neurosurgical expertise and ongoing patient management. Efforts will be needed to ensure equitable access to this advanced therapy.
Further Research and Optimization
Beyond clinical trials, ongoing research will focus on refining patient selection criteria, identifying optimal stimulation targets for different symptom profiles, and exploring personalized approaches to DBS programming. Scientists will also delve deeper into the neurobiological changes induced by DBS to fully understand its therapeutic mechanisms and potentially uncover biomarkers that predict treatment response. The potential implications for other severe psychiatric conditions, such as severe bipolar disorder or treatment-resistant depression with psychotic features, will also be explored.
The pioneering work by Israeli scientists marks a pivotal moment in the fight against schizophrenia. By harnessing the precision of deep-brain stimulation, they are not just treating symptoms, but offering a genuine prospect of reclaiming lives from the grip of a devastating illness.